By Joanne P. Shelby-Klein BSN RN
 Chronic Kidney Disease may continue to progress to the point where the kidneys are unable to filter enough of the waste products and excess fluid causing a build-up of fluid and toxins in the body. When this happens a person is said to have Kidney Failure. When the kidney function decreases to less than 10% the person is considered to have End Stage Renal (kidney) Disease (ESRD) and will need to begin some form of treatment to replace the kidney function or face death. The CDC has reported that in 2011 113,136 patients started some form of treatment for ESRD.
Chronic Kidney Disease may continue to progress to the point where the kidneys are unable to filter enough of the waste products and excess fluid causing a build-up of fluid and toxins in the body. When this happens a person is said to have Kidney Failure. When the kidney function decreases to less than 10% the person is considered to have End Stage Renal (kidney) Disease (ESRD) and will need to begin some form of treatment to replace the kidney function or face death. The CDC has reported that in 2011 113,136 patients started some form of treatment for ESRD.
WHAT HAPPENS WHEN THE KIDNEYS FAIL?
As kidney function continues to decline, patients will be referred to a nephrologist, a doctor who specializes in caring for the kidneys. Ideally, before reaching End Stage, the doctor and patient will discuss the treatment options available to replace normal kidney function. This should happen weeks or months before actual treatment begins so the patient and family have time to decide which treatment is preferable to them. Some nephrologists will refer patients and families to a Treatment Option Educator who is either a Renal Social Worker or Registered Nurse.
WHAT IS RENAL REPLACEMENT THERAPY OR DIALYSIS?
Renal Replacement Therapy or Dialysis is used to remove the excess fluid and waste products from the blood. It does not replace other important healthy kidney functions such as producing vitamin D for healthy bones and erythropoietin to make red blood cells. What Dialysis does is use an artificial process to remove waste products and excess water from the body. The process involves using a semi-permeable (it allows some items to pass through, while keeping others back) membrane to act as a filter and a specially treated solution known as Dialysate to surround the filter. There are two different types of dialysis available; Hemodialysis and Peritoneal Dialysis. Both use the same principle, but each works differently and offers advantages and disadvantages to patients. We will look at each separately.
HEMODIALYSIS
Hemodialysis is the most common type of dialysis used to treat End Stage Renal Disease. It involves the use of a dialysis machine to pump about 200 milliliter of blood per minute from the patient’s body through an artificial kidney (dialyzer) to clean the waste products and excess water and return it to the patient. It requires a blood pump, a dialyzer or artificial kidney, dialysate or washing fluid, and access to the blood for the procedure to occur.
WHAT IS A DIALYZER?
A dialyzer is also known as an artificial kidney. It contains thin fibers that act as the filter for the blood. The dialyzer has two compartments, separated by a thin semi-permeable membrane, one compartment to carry the blood and the other to carry the dialysate. The thin membrane fibers not only separate the blood and dialysate, it also acts as the filter and allows waste products such as urea, creatinine and potassium to be removed from the blood and washed out with the dialysate, while keeping important things like blood cells and proteins in the blood.
As the blood is pumped through the dialyzer in a downward direction, dialysate is pumped in the opposite direction, surrounding the fibers and pulling the waste products and excess fluid from the blood. The blood is returned to the body cleaned and the dialysate is washed down a drain. This process is repeated over several hours to assure that the blood is cleaned many times over. The dialysate used as a washing fluid contains no urea nitrogen or creatinine so that these items can be removed in large quantities. It does contain small amounts of Sodium, Potassium and other electrolytes, mixed with sterile water that the body needs to keep at specific level in order to survive.
HOW DOES THE BLOOD GET FROM THE BODY INTO THE DIALYZER?
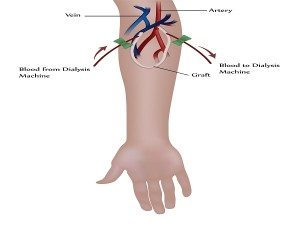
Since Hemodialysis needs a continuous supply of blood moving to and from the patient, there needs to be an access created into one of the veins that can remove the blood safely and return it as the body’s own natural veins are too small to take the repeated needle sticks. Before time for the dialysis treatment to start, ideally several weeks to months, an outpatient procedure to create a dialysis access will be scheduled. For the majority of patients, the procedure involves joining an artery and a vein together to divert some of the arteries blood supply into an adjoining vein through what is called an anastomosis. The blood from the artery is under very high pressure and serves to strengthen the weaker walled vein. This creates a much larger vein that can tolerate having two large needles inserted for each dialysis treatment. However some patients have very poor veins and cannot have this access created. In that case, a central dialysis catheter may be placed, usually in the neck. The picture below shows what each access type looks like.
HOW LONG DOES IT TAKE TO DO A HEMODIALYSIS TREATMENT?
It depends. There are three types of hemodialysis currently available depending on where the treatment is done.
- In-center Hemodialysis. In-center Hemodialysis is the most common type. This is where a patient goes to an outpatient Dialysis Center 3 times a week for a 3 to 4 hour treatment each time. Specially trained nurses and dialysis technicians are there to insert the needles, set up the machines and monitor patients. In-center hemodialysis also offers the opportunity for patients to talk to and offer support to each other. The big disadvantage is that patients are scheduled Monday, Wednesday and Friday or Tuesday, Thursday, Saturday causing some patients to feel that they no longer have control over their schedules.
- Home Hemodialysis. To do home hemodialysis, the patient and a caregiver partner receive training to perform the dialysis treatments at home. They learn how to set-up the machine, insert the needles, monitor the treatment, troubleshoot any problems and discontinue treatments. After approximately 6 weeks of training at the clinic, they go home to perform the treatment for 3-4 hours 3 times a week as if they were in a center. Once a month they see the doctor and training nurse at the clinic to evaluate their treatments and obtain bloodwork. In the event of a machine problem at home the patient can always return to the dialysis center for ongoing treatment. This offers an advantage of the patient deciding what times the dialysis will be completed
- Short Daily Home Hemodialysis. Newer types of dialysis machines now allow patients and their caregiver/partner to do their own dialysis at home on a daily basis. After several weeks of training, the patient can then do treatments 5 to 7 days a week for about 2 hours per treatment. This offers an advantage to some patients because the water and waste product removal is removed on a daily basis, helping to minimize cramping, nausea and vomiting, some of the common side effects of dialysis.
- Nocturnal Home Hemodialysis. After the training period is complete, patients can do their hemodialysis overnight while they sleep. These treatments last for 6 to 8 hours and may be done every other night or six nights a week, depending on the needs of the patient.
The more frequent forms of hemodialysis offer many advantages to patients, including better waste product and fluid removal as well as minimizing the side effects of dialysis such as cramping, nausea and tiredness. Unfortunately, not all dialysis centers offer home hemodialysis as a treatment option because it requires a specially trained nurse to teach the patient and partner, as well as a readily available dialysis machine and station in the event the home dialysis machine is not working.
ARE THERE OTHER FORMS OF DIALYSIS AVAILABLE BESIDES HEMODIALYSIS?
Yes, there is another dialysis treatment option for patients known as Peritoneal Dialysis. Peritoneal Dialysis works along the same principles of Hemodialysis. Blood passes through a semi-permeable membrane that is bathed in dialysate for the blood to be filtered. The difference is in Peritoneal Dialysis the blood does not pass outside the body. Instead it is pumped , by the heart, on its normal course through the abdomen and the organs contained there-in including the semi-permeable peritoneal membrane which covers the organs. If Dialysate or dialysis washing fluid is present in the abdomen, filtering of the blood can occur. If a patient chooses peritoneal dialysis as their treatment option, they need to have a way for the dialysate to get into the abdomen and come in contact with the blood. These patients will have a peritoneal dialysis catheter inserted into their abdomen, either to the right or left of the belly button. This catheter is about the diameter of a small pencil and is approximately 16 inches long. About one half of the catheter is inside the abdomen while the remaining portion is outside. The catheter is held in place by a Velcro cuff that is just under the skin. Once the catheter is healed the training for peritoneal dialysis can begin.
HOW DOES PERITONEAL DIALYSIS WORK?
Peritoneal Dialysis works by exchanging the waste-laden dialysate for fresh dialysate. The process begins by connecting to a sterile tubing set that has an empty drain bag and new dialysate bag. The patient first drains the dialysate that has been sitting in the abdomen, known as dwelling phase, into the empty bag. This process lasts about 20-30 minutes as the bag drains by gravity. Once the drain bag is full it is clamped closed and the new Dialysate solution bag is opened to allow the abdomen to refill with fluid. This takes about 5 to 10 minutes. Once the new bag is completely empty, the patient then closes off the tubing and places a sterile cap on the end of the catheter. The new solution then dwells in the abdomen, while the patient continues with normal daily activities. This process of drain, fill and dwell is repeat several times during the day every day of the week. There are two different types of Peritoneal Dialysis currently available as options.
- CAPD: Continuous Ambulatory Peritoneal Dialysis is done 4 times per day 7 days per week. This is the manual form of dialysis and does not require a machine. Typically the dialysate is left to dwell in the abdomen for 4 to 6 hours during the day and 8 to 10 hours overnight. This allows the patient to have flexibility to schedule the drain and fill portion of the cycle around their own schedule.
- APD: Automated Peritoneal Dialysis. This type of dialysis uses a small machine called a cycler to do the drain and fill cycles over night while the patient sleeps. The patient sets the machine up and connects before going to bed. The machine does the drain, fill and dwell cycles automatically at preset intervals so the patient can have an uninterrupted night sleep. Some patients may combine this type of dialysis with a manual procedure one time midday. The typical dwell time for patients on APD is between 1 to 3 hours depending on patient need.
WHY DON’T MORE PATIENTS DO PERITONEAL DIALYSIS AT HOME?
Peritoneal Dialysis uses the body’s own peritoneal membrane as the filter for the fluid and waste product removal. If the peritoneal membrane has been damaged by multiple surgeries, infections or scar tissue, there may not be enough of the membrane to adequately remove the fluid and waste products putting the patient at risk for a build- up in the blood. People who are morbidly obese are also not recommended for this type of dialysis. Some patients may also not have enough room in their home for the supplies needed to do the dialysis as the supplies are delivered on a monthly basis. Also, some patients may have other medical issues and handicaps that may require a partner to assist in the procedure and the partner is not available.
One of the main reasons there are not more patients on Peritoneal Dialysis is the risk of an infection known as Peritonitis. Peritonitis occurs when the peritoneal membrane and abdomen get bacteria in the normally sterile environment, usually as a result of bacteria getting in when the tubing connection is made. Patients who have tried Peritoneal Dialysis and get peritonitis frequently often have to transfer to Hemodialysis.
IS THERE ANY OTHER TYPE OF DIALYSIS TREATMENT AVAILABLE?
Currently hemodialysis and peritoneal dialysis are the only two dialysis treatments available. In order to decide which is best for each patient, doctors will have a potential patient meet with an educator to discuss the advantages and disadvantages of each type. There is also ongoing research into other dialysis options. In Part 3 of this series we will look at what the future may hold for patients whose kidneys have failed.
References
- Goovaerts, T. Isnard, CB. Crepaldi, C. Dean, J. Melander, S. Mooney, A. Prieto-Melasco, M. Trujillo, C. Zambon, R. Nilsson, EL. (2015) Continuing Education: Preparing Patients to Choose a Renal Replacement Therapy. Journal of Renal Care. Volume 41, Issue 1, pages 62–75, March 2015.
- Rabindranath KS, Adams J, Ali TZ, MacLeod AM, Vale L, Cody JD, Wallace SA, Daly C. Continuous ambulatory peritoneal dialysis versus automated peritoneal dialysis for end-stage renal disease. Cochrane Database of Systematic Reviews 2007, Issue 2. Art. No.: CD006515. DOI: 10.1002/14651858.CD006515
- Smart NA, Dieberg G, Ladhani M, Titus T. Early referral to specialist nephrology services for preventing the progression to end-stage kidney disease. Cochrane Database of Systematic Reviews 2014, Issue 6. Art. No.: CD007333. DOI: 10.1002/14651858.CD007333.pub2.McMillan, J. MD. (2014) Hemodialysis (Intermittent Hemodialysis). Merck Manual Professional Version. https://www.merckmanuals.com/professional/genitourinary-disorders/renal-replacement-therapy/hemodialysis
McMillan, J MD. (2014) Peritoneal Dialysis. Merck Manual Professional Version. https://www.merckmanuals.com/professional/genitourinary-disorders/renal-replacement-therapy/peritoneal-dialysis
- Gayle Hall, BSN, RN, CNN.David Walz, MBA, RN, BSN, CNN.Glenda Payne, MS, RN, CNN. Debra Castner, MSN, RN, CNN.Anna Howard.Kathleen Smith, BS, RN, CNN. (2013). End Stage Renal Disease Briefing Book For State and Federal Policymakers A Guide to Kidney Disease Awareness and Education. American Nephrology Nursing Association. May 2013.
- Nordqvist, C. (2014 September) What is Dialysis? What is Kidney Dialysis? Medical News Today. MediLexicon, Intl., 5 Sep. 2014. Web.30 May. 2015. http://www.medicalnewstoday.com/articles/152902.php
National Kidney Foundation. (2015)
Online Images Courtesy of:
- http://www.webdicine.com/dialysis-diet.html/hemodialysis
- http://classes.kumc.edu/cahe/respcared/cybercas/dialysis/frantype.html
- http://www.joacp.org/viewimage.asp?img=JAnaesthClinPharmacol_2012_28_3_386_98357_u4.jpg
- http://www.renalresource.com/booklets/intropd.php
- http://www.niddk.nih.gov/health-information/health-topics/kidney-disease/peritoneal-dialysis/Pages/facts.aspx